What is an Evaluation of ICP Changes?
Intracranial Pressure (ICP) is the pressure inside the skull, which has a direct effect on the blood perfusion of the brain.
Cerebral Perfusion Pressure (CPP) is a function of the difference between the Mean Arterial Pressure (MAP), which is the driving pressure, and the opposing pressure, which is the ICP:
Optimal CPP is defined as a pressure ≥70 mmHg [2].
How to use TCD for ICP Evaluation
Timely assessment of increased intracranial pressure (ICP) is critical, as it may lead to decreased cerebral perfusion and ultimately to cerebral arrest or brain death. Direct measurements of the intracranial pressure require invasive and potentially harmful clinical procedures, which cannot be applied to every patient. Transcranial Doppler (TCD) is found to be a simple and non-invasive method to assess changes or trends in ICP elevation. The reason to use TCD is primarily due to the fact that increased ICP leads to elevated distal resistance to flow, which in turn has a direct effect on the dynamics of the cerebral blood flow velocity and particularly on the pulsatility indices.
Normally, the brain is a low resistance system with a well-developed autoregulatory capacity and a good collateral protection network designed to ensure proper blood supply to the brain. When ICP starts to increase, the resistance of the brain vasculature starts to increase, and once the autoregulation is exhausted, end-diastolic velocities (EDV) are the first to be affected.
The initial changes with elevated ICP are a decrease in EDV and, in parallel, an increase in the Pulsatility index (PI) and the Resistance Index (RI). With further increase in ICP and the corresponding distal resistance to flow, EDV will be abolished completely and even become oscillating with a negative component. Peak and Mean flow velocity will also decrease correspondingly. Ultimately, when Cerebral Perfusion Pressure (CPP) becomes roughly zero with a further increase in ICP, cerebral perfusion is abolished.

2 MHz Doppler Probe
High quality and ultra sensitive Doppler probe

Monitoring Headset
Perform PFO Test Bilaterally

Robotic Probe
Fast, Stable, and Comfortable Monitoring
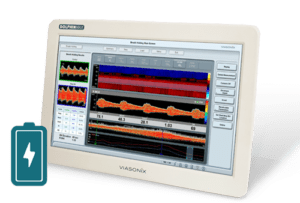
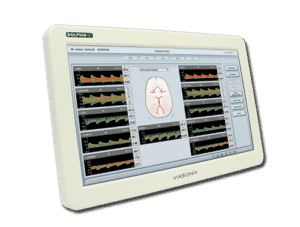
Using the Dolphin for ICP Evaluation
The Dolphin is designed to perform both immediate cerebral flow assessment as well as monitoring to evaluate trends in blood flow dynamics. A wide selection of parameters that define the blood flow velocity is available, including Peak, Mean, and End-Diastolic Velocities, and a range of pulsatility indices: PI (Pulsatility Index), RI (Resistance Index), and S/D (Systolic to Diastolic Ratio). In addition, systolic rise time (RT) and the heart rate (HR) are provided and can be continuously monitored.
When patient examinations are performed periodically over the course of hospitalization, the Dolphin allows the trending of any selected parameter at any selected blood vessel in order to determine the suspected changes in ICP and perform a timely clinical intervention prior to brain damage or arrest.
In addition, with the aid of the dedicated Dolphin monitoring headframe or the unique Dolphin/XF TCD robot, bilateral monitoring of the cerebral flow allows continuous assessment of potential ICP changes and timely identification when blood flow dynamics begin to suggest a dangerous increase in ICP. Any of the velocity or pulsatility parameters can be trended, and markers can be added to identify special events such as medication or other medical procedures.
Expected Results
CPP is the difference between the driving arterial pressure and the opposing intracranial pressure.
Thus, when ICP starts to increase beyond the diastolic pressure, a retrograde flow component may be seen in the blood flow velocity waveform, with a tri-phasic like dynamics. Alternatively, the increase in ICP may lead to a sharp increase in systolic flow and an absent end-diastolic flow. High resistance waveforms are seen with PI ≥ 1.2. A further increase in ICP could lead to cerebral arrest leading to Brain Death.
Selected Literature
Transcranial Doppler Monitoring of Intracranial Pressure Plateau Waves, Danilo Cardim et al., Neurocrit Care (2017) 26:330–338
The Role of Transcranial Doppler in Traumatic Brain Injury: A Systemic Review and Meta‑Analysis, Nida Fatima et al., Asian J Neurosurg 2019;14:626-33
Non-invasive Monitoring of Intracranial Pressure Using Transcranial Doppler Ultrasonography: Is It Possible?, Danilo Cardim et al., Neurocrit Care (2016) 25:473–491
Transcranial Doppler: Techniques and advanced applications: Part 2, Sharma AK, Bathala L, Batra A, Mehndiratta MM, Sharma VK, Ann Indian Acad Neurol. 2016 Jan-Mar;19(1):102-7
Transcranial Doppler ultrasonography in anaesthesia and intensive care, I. K. Moppett and R. P. Mahajan, British Journal of Anaesthesia 93 (5): 710–24 (2004)
Transcranial Doppler, Peter J. Kirkpatrick and Kwan-Hon Chan, Chapter 13, in Head Injury. Edited by Peter Reilly and Ross Bullock. Published in 1997 by Chapman & Hall, London
Neuro-ultrasonography, Ryan Hakimi, Andrei V. Alexandrov, and Zsolt Garami, Neurol Clin 38 (2020) 215–229
Transcranial Doppler, Review Article, Manish K. Marda, Hemanshu Prabhakar, J Neuroanaesthesiol Crit Care 2015;2:215-20
Assessment: transcranial Doppler ultrasonography: Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Sloan MA et al., Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology. 2004 May 11;62(9):1468-81
Disclaimer of Information & Content
The content of Viasonix Ltd. website is for information only, not advice or guarantee of outcome. Information is gathered and shared from reputable sources; however, Viasonix Ltd. Management is not responsible for errors or omissions in reporting or explanation. No individuals, including those under our active care, should use the information, resources or tools contained within this self-diagnosis or self-treat any health-related condition. Viasonix Ltd. Management gives no assurance or warranty regarding the accuracy, timeliness or applicability or the content.