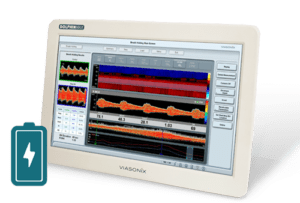
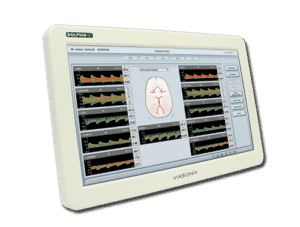
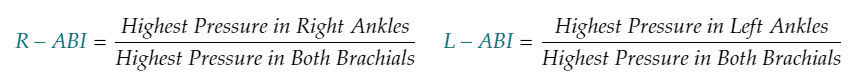What is Ankle Brachial Index (ABI)?
Ankle Brachial Index (ABI) test assists in the early detection of Peripheral Arterial Disease (PAD) and provides information about its functional severity.
During the ABI test, the primary Systolic pressures are measured in each of the right and left brachials, as well as at the level of the right and left ankles.
Ankle Brachial Index, or ABI, is determined as the ratio between the higher brachial systolic pressure and each of the ankle pressures. Thus, a separate ABI value is obtained for the Right side and the Left sides (3).
Unlike ultrasound imaging modalities which provide anatomical information, ABI assessment provides a direct indication of the physiological severity of the vascular pathology, such as Peripheral Arterial Disease. ABI testing machines are often used for fast and simple screening of the lower limbs, prior to determining if ultrasound imaging is required (1,4).
Common Indications Often Used for an ABI Test
Common Indications
Common indications for an ABI test span clinical presentations like leg pain, cramping, or numbness experienced during exercise—symptoms of a condition termed intermittent claudication.
Non Healing Wounds
Persistent, non-healing wounds on the lower extremities can also signify compromised blood circulation, necessitating an ABI evaluation.
Peripheral Arterial Disease Symptoms
Peripheral arterial disease and its associated symptoms also direct clinicians towards ABI as an essential initial diagnostic measure.
Post-Operative Settings
Importantly, ABI also finds application in post-operative settings. Following vascular procedures, ABI serves as a monitoring tool, helping to track the success of interventions and the patient’s progress during recovery. It aids in identifying potential complications and ensuring that surgical objectives, such as improved blood flow, are achieved. In this context, the ABI test remains an invaluable asset in the repertoire of vascular specialists, often deployed as a frontline diagnostic and monitoring measure prior to using more complicated imaging or further interventions.
How to Perform Ankle Brachial Index Test?
This step-by-step guide focuses on measuring ABI using a Doppler probe, the most clinically accepted method. Although photoplethysmography (PPG) and oscillometry can also be used, they are often considered less accurate than the gold standard Doppler method.
Step 1: Patient History and Preparation
- Begin by taking a thorough medical history of the patient, noting any risk factors for peripheral artery disease such as smoking, diabetes, and hypertension.
- Ensure the patient is in a comfortable supine position and has rested for at least 10 minutes before the test to stabilize peripheral circulatory conditions.
- Use an ABI machine with Doppler functionality and blood pressure cuffs. For improved accuracy, the ABI machine, at a minimum, needs to show a color-coded spectral waveform and a pressure curve representing the pressure in the cuff during the inflation/deflation period.
- Preferably, use an 8 MHz Doppler probe, which is ideal for most peripheral vascular arteries due to its balance between depth and resolution.
Step 2: Test Environment and Cuff Placement
- The test should be conducted in a warm environment to prevent vasoconstriction, which may affect results.
- Place the blood pressure cuffs on both brachials and ankles. The cuffs should be snug but not too tight to avoid distorting the pressure readings.
Step 3: Brachial Pressures Measurements
- Start by measuring the systolic blood pressure at the right and left brachials.
- Position the 8 MHz Doppler probe distal to the pressure cuff on the upper extremity and angle it at 45-60 degrees to the radial/ulnar blood vessels near the wrist.
- Inflate the cuff until the Doppler signal disappears and then slowly deflate it. The pressure at which the Doppler signal reappears is the systolic blood pressure.
- Record the highest systolic pressure obtained from either brachial of each hand, along with the quality of the Doppler signals.
Step 4: Ankles Pressure Measurements
- Continue by measuring the systolic blood pressure at the right and left ankles. It is important to take a separate pressure measurement for the dorsalis pedis and posterior tibial of each leg.
- Position the 8 MHz Doppler probe distal to the pressure cuff on the lower extremity and angle it at 45-60 degrees to the dorsalis pedis and posterior tibilal blood vessels near the foot.
- Similarly to the previous step, inflate the cuff until the Doppler signal disappears and then slowly deflate it. The pressure at which the Doppler signal reappears is the systolic blood pressure.
- Follow the same process to measure the systolic blood pressure at the right and left dorsalis pedis and posterior tibial arteries.
- Record the highest systolic pressure obtained from either the dorsalis pedis or posterior tibial artery for each leg, along with the quality of the Doppler signals.
Step 5: Calculating and Interpreting the ABI
- Calculate the ABI for each leg using the formula: ABI = Highest Ankle Systolic Pressure / Highest Brachial Systolic Pressure.
- Compare the ABI values with standard ranges as indicated by public health guidelines.
Step 6: Post-Test Actions
- If the ABI is abnormal or borderline, refer the patient for further diagnostic testing and discuss the results in the context of the patient’s overall cardiovascular risk.
Step 7: Additional Test Extensions (Optional)
- For a more comprehensive evaluation, perform segmental blood pressures by placing cuffs on additional segments of the legs.
- To assess the effect of exercise on ABI, conduct the ABI test before and after a stress activity such as walking or treadmill exercise.
- For patients with non-compressible arteries, toe-brachial index (TBI) or pulse volume recording (PVR) may be considered.
This step-by-step guide for performing an Ankle Brachial Index test is for informational purposes only. Healthcare professionals should rely on their expertise, clinical judgment, and institutional protocols for accurate administration and interpretation. Additional clinical information, patient history, physical examination, and other diagnostic tests may be necessary for comprehensive evaluation.
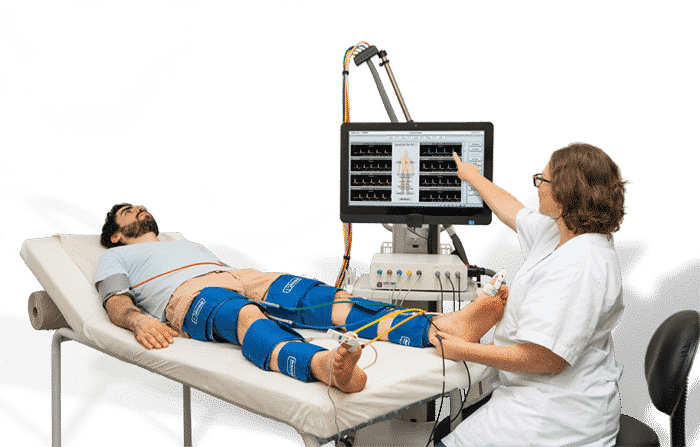
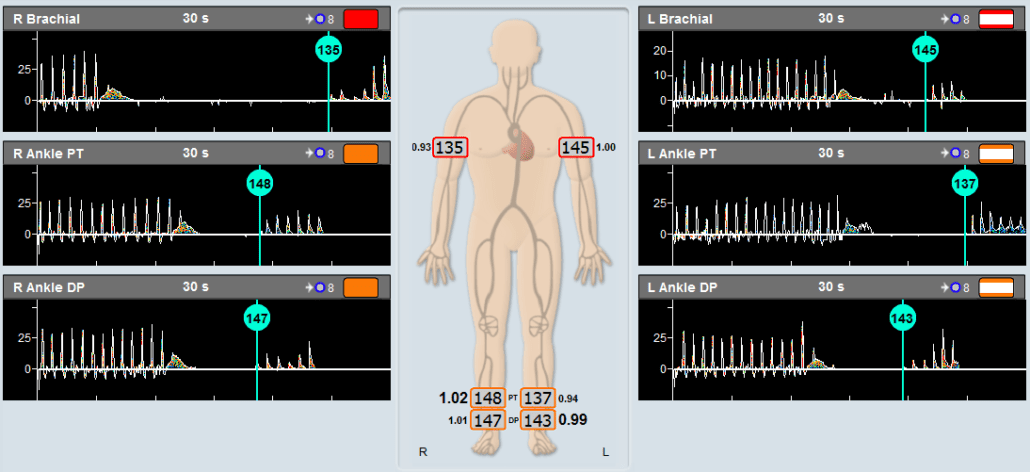
Example of an ABI test performed on a patient using Viasonix Falcon/PRO ABI Doppler machine. The sensor used in this case is 8 MHz Doppler probe.
What is the Most Clinically Accepted ABI Test Method?
Using Doppler to measure the distal waveform is the traditional and clinically accepted method (1). Usually, ABI is calculated at both Dorsalis Pedis Artery and Posterior Tibial Artery. The higher ABI on each side is then taken as the final result to assess Peripheral Arterial Disease (PAD) severity in each leg (1, 2, 3, 4).
ABI Test Reimbursement Considerations
Doppler measurement is the recommended clinical method to receive full reimbursement on CPT codes 93922, 93923, and 93924. The different codes differ in their level of complexity, but all are based on the ABI Doppler method.
Other methods for testing ABI are Photoplethysmograph (PPG) sensors and Oscillometric devices. Both are considered less accurate than the Doppler, especially under challenging conditions, which is probably why these methods are not reimbursable under CPT Codes 9392#.
Receiving full reimbursement for this test, especially for CPT Code 93924, may prove difficult or impossible with less accurate methods such as PPG, Oscillometry, or Automated ABPI. The accepted method requires a diagnostic device such as the Falcon/PRO that provides integrated protocols and reporting for ABI on both Dorsalis Pedis and Posterior Tibial, Segmental Blood Pressures, and Treadmill test.
Using the Falcon for ABI Measurements
The Falcon is considered to be the best ankle brachial index machine as it allows very simple and fast diagnosis of ABI. Simply place 4 color-coded pressure cuffs on each of the right/left brachial and ankle sites, select the ABI protocol, and you are ready to go. The ABI test can be completed in just a couple of minutes.
Simple and Fast Diagnosis
The Falcon is designed to provide a straightforward and efficient ABI test. With its user-friendly interface and color-coded pressure cuffs, Doppler probes and PPG sensors, examiners can easily perform the test and obtain results quickly. This simplicity allows for streamlined workflow and reduces the testing time for patients.
Systolic Pressure Cursor
Once the distal Doppler or PPG waveform reappears during the deflation phase of the pressure cuff, the measurement can be stopped, and the Falcon places a cursor to mark a potential systolic pressure. The user may move the cursor to a different location to change the systolic pressure as needed. Right/Left ABI values are calculated automatically by the Falcon and presented clearly on the screen and in the report layout.
Wide Range of Doppler Probes and PPG Sensors
The Falcon is also known as a peripheral vascular diagnosis system as it allows you to select from a wide variety of Doppler probes and Photoplethysmograph (PPG) sensors for best outcome. This flexibility enhances the test to help achieve high-quality results.
Customizable Parameters
The Falcon allows users to customize various parameters, such as target inflation pressure and deflate rate, to suit individual patient requirements.
Automatic Cuff Inflation and Signal Identification
The Falcon is equipped with advanced features, such as automatic cuff inflation once a signal is identified and simultaneous measurements, which further simplify the testing process. These features enable a more efficient workflow and reduce the potential for human error.
Contralateral Results Display
The Falcon can display results from both the right and left sides simultaneously, allowing clinicians to compare and analyze the ABI values more effectively. This feature has the potential for better diagnosing and evaluating Peripheral Arterial Disease (PAD) severity in each leg.
Clear Reporting and Data Presentation
The Falcon presents ABI values clearly on the screen and generates a detailed report layout. The comprehensive report provides valuable information for healthcare professionals.
Gold Standard Doppler Method
The Falcon uses Doppler to measure the distal waveform, which is the accepted method for ABI testing. Doppler provides higher accuracy compared to other methods, such as PPG sensors and oscillometric devices, especially under challenging conditions (7).
Enhanced Peripheral Vascular Diagnosis System
Beyond ABI testing, the Falcon serves as a versatile peripheral vascular diagnosis system. It can perform additional tests like Segmental Blood Pressures, Toe Brachial Index, Treadmill Test, Pulse Volume Recording, and more, expanding its capabilities for comprehensive vascular assessment.
Expected Results of ABI Test
| Range | Common Diagnosis |
|---|---|
| ABI ≥ 1.4 | Non compressible arteries |
| 1 ≤ ABI < 1.4 | Normal |
| 0.9 ≤ ABI < 1 | Borderline |
| ABI ≤ 0.9 | Abnormal |
Clinical Correlation
It’s important to correlate ABI results with the patient’s symptoms and clinical presentation. Some patients with an ABI in the normal range may still have PAD, especially if they have atypical symptoms or other risk factors (2).
Severity Assessment
An ABI ratio of around 1 is considered normal, while lower values indicate various levels of significant peripheral arterial disease (PAD) and higher ABI values represent incompressible arteries which are typically associated with higher vascular stiffness. Borderline results may warrant further evaluation and monitoring (2).
Bilateral Comparison
Compare the ABI values between the right and left sides. A significant difference in ABI values (more than 0.15) between the two sides or a pressure difference greater than 20 mmHg between the bilateral leg segments may suggest unilateral disease or arterial occlusion (3).
Other Diagnostic Tests
ABI is a screening test, and further investigations may be needed to confirm the diagnosis or assess the extent of arterial disease. Additional tests may include Segmental Blood Pressures, Pulse Volume Recording, and Treadmill Exercise Test, Toe Brachial Index (TBI), among others.
Consultation
Interpreting ABI results and making clinical decisions based on them should be done by a qualified healthcare professional experienced in vascular diagnosis and management.
Selected Literature for Ankle Brachial Index Testing
- Overview of Peripheral Arterial Disease of the Lower Extremity, Ali F. AbuRahma and John E. Campbell, Noninvasive Vascular Diagnosis, A.F. AbuRahma (ed.), Springer International Publishing AG 2017, Ch 21, pp 291-318
- 2016 AHA/ACC Guideline on the Management of Patients With Lower Extremity Peripheral Artery Disease; A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines; Journal of the American College of Cardiology, Vol. 69, No. 11, 2017
- Peripheral vascular disease assessment in the lower limb: a review of current and emerging non‑invasive diagnostic methods, Shabani Varaki et al, BioMed Eng OnLine (2018) 17:61
- 2017 ESC Guidelines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in collaboration with the European Society for Vascular Surgery (ESVS), Victor Aboyans et al., European Heart Journal (2017) 00, 1–60
- The Ability of the Toe-Brachial Index to Predict the Outcome of Treadmill Exercise Testing in Patients with a Normal Resting Ankle-Brachial Index, Christian Høyer et al, Annals of Vascular Surgery, Volume 64, April 2020, Pages 263-269
- Association of cardiovascular autonomic dysfunction with peripheral arterial stiffness in patients with type 1 diabetes, Lía Nattero-Chávez et al, The Journal of Clinical Endocrinology & Metabolism
- Measurement and Interpretation of the Ankle-Brachial Index, Victor Aboyans et al, Circulation. 2012;126:2890–2909
- The effect of percutaneous transluminal angioplasty of superficial femoral artery on pulse wave features, Mikko Peltokangas et al, Computers in Biology and Medicine 96 (2018) 274–282
Disclaimer of Information & Content
The content of Viasonix Ltd. website is for information only, not advice or guarantee of outcome. Information is gathered and shared from reputable sources; however, Viasonix Ltd. Management is not responsible for errors or omissions in reporting or explanation. No individuals, including those under our active care, should use the information, resources or tools contained within this self-diagnosis or self-treat any health-related condition. Viasonix Ltd. Management gives no assurance or warranty regarding the accuracy, timeliness or applicability or the content.