What is Toe Brachial Index?
The Toe Brachial Index (TBI) is defined as the ratio between the systolic blood pressure in the right or left toe and the higher of the systolic pressure in the right or left arms.

TBI is a common vascular physiologic assessment test taken to determine the existence and severity of peripheral arterial disease (PAD) in the lower extremities.
A peripheral arterial disease in the lower extremities happens when the blood vessels in the legs or towards the legs are narrowed or blocked. This most commonly occurs due to atherosclerosis, which is a thickening or hardening of the arteries as a result of fatty plaque building up in the arteries. PAD can also happen in the arms, but it is most common in the legs.
When is a TBI Test Recommended?
The TBI test is most often recommended by a doctor when a patient has symptoms of PAD such as pain, numbness, or fatigue in the feet or legs. It is also sometimes recommended if the patient has risk factors for PAD such as high blood pressure, high cholesterol, or diabetes.
Frequently, Toe-Brachial Index (TBI) is a complementary measurement to the ABI (Ankle-Brachial Index) test. It is especially useful when the ABI cannot be measured, if it is inconclusive, or if it is abnormally high, for example, in diabetic patients.
Early detection of PAD is critical. If left untreated, it may lead to a Critical Limb Ischemia (CLI). In this condition, severe blockages in the lower extremity arteries prevent enough oxygenated blood from reaching the legs. This poor circulation may result in leg pain, claudication, and in severe cases even Gangrene (broken and dead tissue) and a need for amputation.
TBI measurements are fast, simple, non-invasive, and painless and are widely popular to assist in the early detection of Peripheral Artery Disease.
Toe Measurement using a Digit Blood Pressure Cuff and a PPG Sensor
What is ABI and TBI test?
ABI tests have an important role in diagnosing peripheral arterial disease.
The TBI measurements in the right/left toes are often taken if the ABI measurements are high (for example, above 1.3) or if the ankle’s arteries are determined as incompressible when measuring the ABI.
While the Ankle Brachial Index measurement can become unreliable when arterial stiffness increases, the Toe Brachial Index is less susceptible to vascular stiffness. This distinction is because an important characteristic of the digit or toe arteries is that they usually do not calcify and therefore do not have increased vascular stiffness.
Thus, the TBI is a valuable diagnostic tool when the blood vessels are stiff or incompressible, as may be the case, for example, when diagnosing patients with Diabetes Mellitus (DM).
How to Measure Toe Brachial Index
Measuring the TBI as part of Peripheral Arterial Disease (PAD) evaluation is fast and simple.
The test is typically performed by a doctor or other healthcare professional in a medical setting:
- In preparation for the test, wrap a toe/digit blood pressure cuff around the measured toe.
- Use blood pressure cuffs in a size that is suitable for the toe.
- Place a sensor, normally a Photoplethysmograph (PPG) sensor based on infrared light, on the toe distally to the small blood pressure cuff. In some special cases, you can use a Doppler measurement instead of the PPG measurement to perform the test.
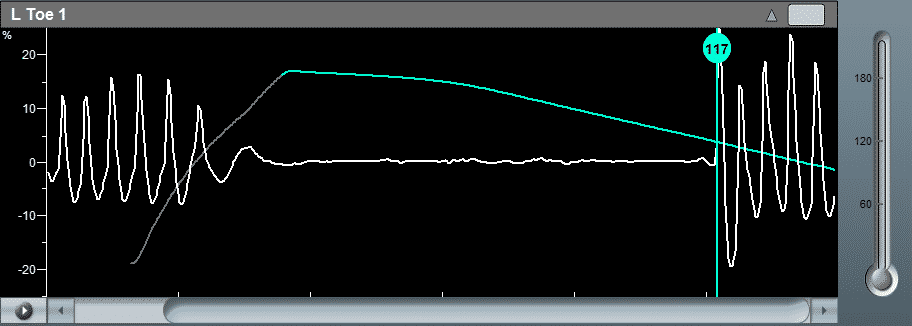
- Inflate the toe pressure cuff above normal systolic blood pressure until the distal PPG signal flattens, indicating total arterial occlusion.
- The blood pressure cuff is then deflated in a controlled manner, and the pressure at which the phasic PPG waveform reappears is determined as the systolic pressure.
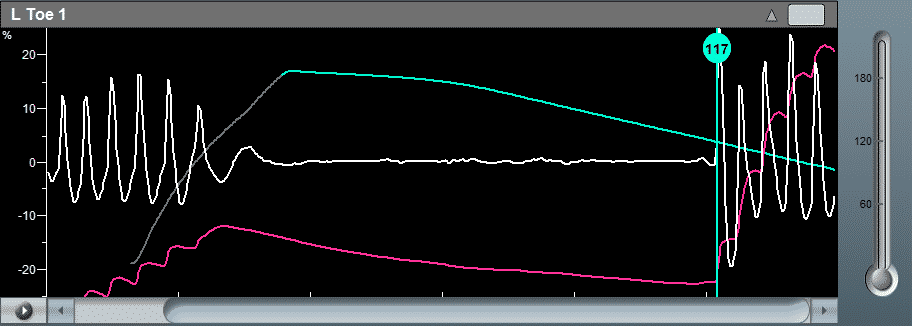
- Due to the noisy PPG signal environment, high-end ABI machines also present the “average” PPG curve (or DC PPG) curve. The average curve tends to rise at the correct systolic return. Using this method, technicians can easily determine the systolic blood pressure location.
- Finally, repeat the process described above for the 2 Brachial segments and for 2 toes.
Toe Measurement with DC PPG Curve
How is the TBI Calculated?
The Toe-Brachial Index (TBI) is calculated as follows:

Usually, an Ankle Brachial Index (ABI) test is also carried out, which means the Brachial segments have already been measured. The highest of the two Brachial systolic pressures is used as a reference.
Using the Falcon for TBI Measurements
The Falcon as a TBI Machine is designed to allow completing the Toe Brachial Index diagnosis in a fast and straightforward manner.
- Efficiency and Simplicity: Streamlined the TBI measurement process, making it fast and straightforward.
- Complete Replay: Ability to review in offline the entire waveform of each measured toe.
- Systolic Pressure Cursor: The Falcon system places a cursor next to the pulse reappearance. You can easily move the cursor to adjust the systolic pressure.
- Advanced Sensor Technology: State-of-the-art and ultra-sensitive Photoplethysmograph (PPG) sensors based on infrared light.
- Multiple Toe Measurements: Simultaneous pressure measurements in up to five separate toes to reduce examination time and easier comparison of toe waveforms.
- Supplementary Criteria: Option to display the “average” (or, “DC”) PPG waveform, which is particularly beneficial in noisy environments in finding the optimal systolic pressure.
- Doppler Option: Using a unique 10 MHz Doppler probe for superficial penetration, in case it is preferred for TBI testing.
- Clear Reporting: Detailed examination reports that includes the TBI indexes and optionally also the waveforms.
- Adaptive Features: Customize various parameters, such as target inflation pressure and deflate rate, for optimal measurements.
- Variety of Sensor Configurations: Including fingerclip PPG sensors for digits or long toes, toe clip PPG sensors for rapid placement, and disk PPG sensors for toes with limited space.
Expected Results for TBI
Although the pathologic TBI criteria are still somewhat ambiguous, a common Toe Brachial Index normal values range is shown in the table below.
| Range | Common Diagnosis |
|---|---|
| TBI ≥ 0.7 | Normal |
| TBI < 0.7 | Abnormal |
Specifically, TBI < 0.7 is considered abnormal and is associated with claudication, and a TBI < 0.2 is associated with pain at rest.
The absolute systolic toe pressure is also an important diagnostic parameter for Peripheral Arterial Disease. A normal toe pressure is about 30 mmHg less than the ankle pressure. A systolic toe pressure of less than 30 to 50 mmHg suggests chronic limb ischemia, according to the recommendations of the TASC group.
A TBI value less than 0.5 suggests proximal arterial disease of moderate severity, while an index less than 0.2 and toe pressures less than 30 mm Hg are consistent with critical ischemia and poor potential for healing.
The TBI normal values are different from the ABI normal values because the toe blood pressures are expected to be less than ankle/brachial blood pressures.
TBI results may vary depending on factors like age and gender. Therefore, a knowledgeable healthcare provider should be consulted to interpret these results.
Selected Literature
Overview of Peripheral Arterial Disease of the Lower Extremity, Ali F. AbuRahma and John E. Campbell, Noninvasive Vascular Diagnosis, A.F. AbuRahma (ed.), Springer International Publishing AG 2017, Ch 21, pp 291-318
2016 AHA/ACC Guideline on the Management of Patients With Lower Extremity Peripheral Artery Disease; A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines; Journal of the American College of Cardiology, Vol. 69, No. 11, 2017
Peripheral vascular disease assessment in the lower limb: a review of current and emerging non‑invasive diagnostic methods, Shabani Varaki et al, BioMed Eng OnLine (2018) 17:61
2017 ESC Guidelines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in collaboration with the European Society for Vascular Surgery (ESVS), Victor Aboyans et al., European Heart Journal (2017) 00, 1–60
The Ability of the Toe-Brachial Index to Predict the Outcome of Treadmill Exercise Testing in Patients with a Normal Resting Ankle-Brachial Index, Christian Høyer et al, Annals of Vascular Surgery, Volume 64, April 2020, Pages 263-269
Association of cardiovascular autonomic dysfunction with peripheral arterial stiffness in patients with type 1 diabetes, Lía Nattero-Chávez et al, The Journal of Clinical Endocrinology & Metabolism
The toe-brachial index in the diagnosis of peripheralarterial disease, Christian Høyer et al, Journal of Vascular Surgery, Volume 58, Issue 1, P231-238, July 01, 2013
Inter Society Consensus Report for the Management of PAD, TASC II report (Trans-Atlantic Inter-Society Consensus), Ed. Lars Norgren and William R Hiatt, The Society for Vascular Surgery, doi:10.1016.
Peripheral vascular disease assessment in the lower limb: a review of current and emerging non‑invasive diagnostic methods; Shabani Varaki et al, BioMed Eng OnLine (2018) 17:61
Disclaimer of Information & Content
The content of Viasonix Ltd. website is for information only, not advice or guarantee of outcome. Information is gathered and shared from reputable sources; however, Viasonix Ltd. Management is not responsible for errors or omissions in reporting or explanation. No individuals, including those under our active care, should use the information, resources or tools contained within this self-diagnosis or self-treat any health-related condition. Viasonix Ltd. Management gives no assurance or warranty regarding the accuracy, timeliness or applicability or the content.