In this session, we will discuss frequently asked questions about the PFO test, also known as “TCD Bubble Study”.
What is a Transcranial Doppler Bubble Study?
A Transcranial Doppler Bubble Study is a diagnostic test that utilizes ultrasound Doppler technology to examine the blood circulation through the blood vessels in the brain.
It is primarily used to detect the presence of a Patent Foramen Ovale (PFO), a heart defect where there is a small opening between the upper chambers of the heart (atria) that should have closed shortly after birth.
Why is a TCD Bubble Study performed?
The TCD Bubble Study is performed to assess the possibility of a PFO and to investigate potential causes of stroke, transient ischemic attack (TIA), or other neurological conditions related to abnormal blood flow between the heart and the brain.
What is a Patent Foramen Ovale (PFO)?
A Patent Foramen Ovale (PFO) is a congenital heart defect characterized by a persistent opening between the atria (upper chambers) of the heart, which should have closed soon after birth.
How does a PFO cause health issues?
A PFO may potentially allow blood clots or substances to pass from the right atrium to the left atrium and then travel to the brain, leading to neurological issues such as stroke or TIA (Transient Ischemic Attack).
How is a Transcranial Doppler Bubble Study performed?
During a Transcranial Doppler Bubble Study, a saline solution with tiny air bubbles is injected into the bloodstream, and a TCD device is used to monitor the movement and behavior of these bubbles in the blood vessels of the brain.
The bubbles appear as emboli in the bloodstream, with very specific characteristics that a professional TCD neurosonologist can easily identify.

Is the TCD Bubble Study a painful procedure?
No, the TCD Bubble Study is a generally painless procedure.
Are there any risks or side effects associated with the TCD Bubble Study?
The TCD Bubble Study is considered safe, and there are typically no significant risks or side effects associated with it. In rare cases, some individuals may experience minor discomfort or bruising at the injection site.
How long does the procedure take?
The TCD Bubble Test usually takes around 30 minutes to an hour to complete.
Can I eat or drink before the test?
Generally, you can eat and drink as usual before the TCD Bubble Study unless your healthcare provider instructs otherwise.
What can I expect during the TCD Bubble Study?
During the TCD Bubble Study, you will usually lie on an examination table, and a healthcare professional will perform the Transcranial Doppler examination and inject the saline solution with the bubbles while monitoring the blood flow in your brain.
Who performs the Transcranial Doppler Bubble Study?
The TCD Bubble Study is usually conducted by a trained medical professional, such as a cardiologist or a neurologist, who specializes in this type of diagnostic procedure.
How long does it take to get the results?
The results of the TCD Bubble Study are typically available shortly after the procedure is completed.
What are the possible interpretations of the test results?
The test results may indicate the presence or absence of a PFO and provide insights into the blood flow patterns and the potential risk of blood clots passing from the heart to the brain. In general, a larger number of detected emboli micro-bubbles that are detected suggest a larger shunt between the right and left heart atriums.
What conditions or disorders does the TCD Bubble Study help diagnose?
The TCD Bubble Study aids in diagnosing PFO, as well as identifying potential causes of stroke, TIA, and other neurological conditions associated with abnormal blood flow between the heart and brain.
Can the TCD Bubble Study detect other neurological conditions?
The TCD Bubble Study primarily focuses on assessing the presence of a PFO and its associated risks. However, measurements of cerebral blood flow velocity are part of routine TCD examinations and may also provide additional information that could help with the evaluation of certain neurological conditions.
Are there any limitations to the test?
While the TCD Bubble Study is a valuable diagnostic tool, it may not detect all cases of PFO or provide a complete assessment of all potential causes of neurological conditions.
Can the TCD Bubble Study be used as a preventative measure?
The TCD Bubble Study is primarily a diagnostic procedure and is not typically used as a preventative measure. However, it can help identify individuals at risk of certain neurological events related to a PFO.
What treatment options are available if a PFO is detected?
Treatment options for a detected PFO depend on the individual’s medical history, symptoms, and associated risks. Some cases may be managed with medication, while others may require surgical or minimally invasive procedures to close the PFO.
How common is a PFO?
A PFO is relatively common and is estimated to be present in about 20-25% of the general population.
Are there any lifestyle changes recommended after a positive TCD Bubble Study?
If a PFO is detected and there is an associated risk of neurological events, lifestyle changes, and preventive measures such as antiplatelet medications may be recommended by your healthcare provider to reduce the risk of complications.
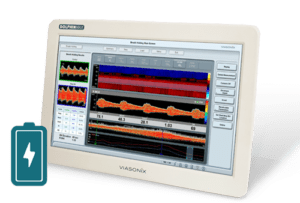
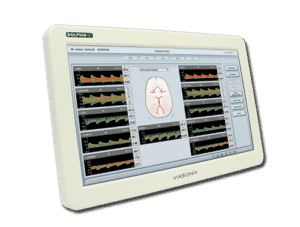
What is the equipment used in Transcranial Doppler Bubble Study (TCD)?
The equipment used in TCD Bubble Study involves a Transcranial Doppler ultrasound machine, a contrast agent (usually saline solution with microbubbles), and a specialized transducer probe. The transducer emits and receives ultrasound waves to assess blood flow in the brain’s blood vessels and detect the presence of bubbles when the contrast agent is introduced.
How does the transcranial Doppler ultrasound machine work in the TCD Bubble Study?
The transcranial Doppler ultrasound machine utilizes Doppler technology to measure the speed and direction of blood flow in the arteries of the brain. It uses high-frequency sound waves that bounce off red blood cells and produce audible signals or waveforms, helping healthcare professionals visualize blood flow patterns and identify abnormalities like a PFO.
What are microbubbles, and why are they used as a contrast agent in the TCD Bubble Study?
Microbubbles are tiny gas-filled bubbles that are mixed with saline solution to create a contrast agent. When injected into a vein, these microbubbles can pass through a PFO and travel directly to the brain. The transcranial Doppler machine can then detect the microbubbles as embolic signals within the blood flow in the brain arteries.
Is the TCD Bubble Study with microbubbles safe?
The TCD Bubble Study with microbubbles is considered generally safe and well-tolerated. The microbubbles typically do not cause harm to the body.
Are there alternative methods to perform the TCD Bubble Study without microbubbles?
Yes, there are alternative methods to perform the TCD Bubble Study without microbubbles. One such method is the Valsalva maneuver technique. During this approach, the patient is asked to perform the Valsalva maneuver, which involves forcefully exhaling while keeping the mouth and nose closed. This maneuver temporarily increases pressure in the chest and may cause a naturally occurring “shunting” of blood through a PFO, enabling its detection during the TCD test.
How does the Valsalva maneuver technique serve as an alternative to microbubbles in the TCD Bubble Study?
The Valsalva maneuver technique serves as an alternative by creating transient changes in pressure within the heart and the chest. This can induce blood flow alterations and facilitate the identification of a PFO without the need for microbubbles.
However, the combination of performing the Valsalva maneuver following the injection of the microbubbles can help in visualizing the embolic shower in the brain arteries.
What other conditions can be assessed using Transcranial Doppler (TCD) besides a PFO?
Transcranial Doppler (TCD) can be used to assess various conditions related to blood flow in the brain, including cerebral vasospasm after subarachnoid hemorrhage, evaluation of intracranial stenosis, monitoring of cerebral blood flow during surgery or critical care, and identification of emboli and other abnormalities in the cerebral circulation.
Can TCD be used to diagnose conditions outside the brain?
While TCD is primarily used to assess cerebral blood flow, it can be adapted to study blood flow in other parts of the body, such as the carotid and vertebral arteries, to evaluate blood flow dynamics and detect certain vascular disorders.
How does Transcranial Doppler differ from other brain imaging techniques like MRI or CT scans?
Transcranial Doppler is a functional technique that assesses blood flow in real time, providing information on blood velocity and patterns. In contrast, MRI and CT scans are structural imaging techniques that visualize brain anatomy and detect abnormalities like tumors, bleeding, or structural defects but may not directly show blood flow dynamics.
Are there alternative methods for determining PFO that are not TCD related?
Transthoracic Echocardiogram (TTE) is a standard echocardiogram that uses ultrasound waves to create images of the heart’s structures. A contrast agent can be injected during the test to visualize the passage of bubbles through a PFO. Transesophageal Echocardiogram (TEE) TEE is another method that involves inserting a specialized ultrasound probe into the esophagus to obtain clearer images of the heart’s structures. With the use of a contrast agent, TEE can help visualize the presence of a PFO and assess its characteristics in more detail.
Please note that medical technology and practices may evolve over time, and it’s always best to consult with a healthcare professional or medical expert for the most up-to-date information regarding TCD instrumentation and alternative methods for the TCD Bubble Study.
What is an embolic shower?
An embolic shower is a medical condition that occurs when multiple emboli (small clots, debris, or micro-bubbles) travel through the bloodstream and lodge in various blood vessels throughout the body or simply pass through the vascular bed.
The term “shower” is used because it describes the scenario where multiple emboli break off from a larger source, such as a blood clot in the heart, atherosclerotic plaque in an artery, or micro-bubbles generated for example during PFO testing.
The embolic shower travels downstream, causing either blockages in smaller blood vessels or in the case of micro-bubbles dissipate while passing through the microcirculation. A embolic shower of solid material is a serious medical emergency and can lead to various complications depending on where the emboli become lodged.
For example, if the emboli obstruct blood flow to the brain, it can lead to a stroke. TCD equipment can easily detect embolic showers to the brain while monitoring the MCA artery.